Inside This Issue
Ultrasound & Deep Learning for PCa Detection
Management of PCa Patients with PSMA-PET
Using Holmium Lasers in Octogenarian PCa Patients
Focal Therapy Using a Cooled Laser Device
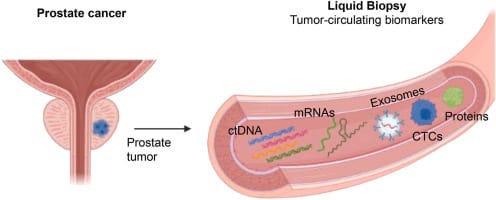
Epigenetic & Liquid Biopsy of PCa
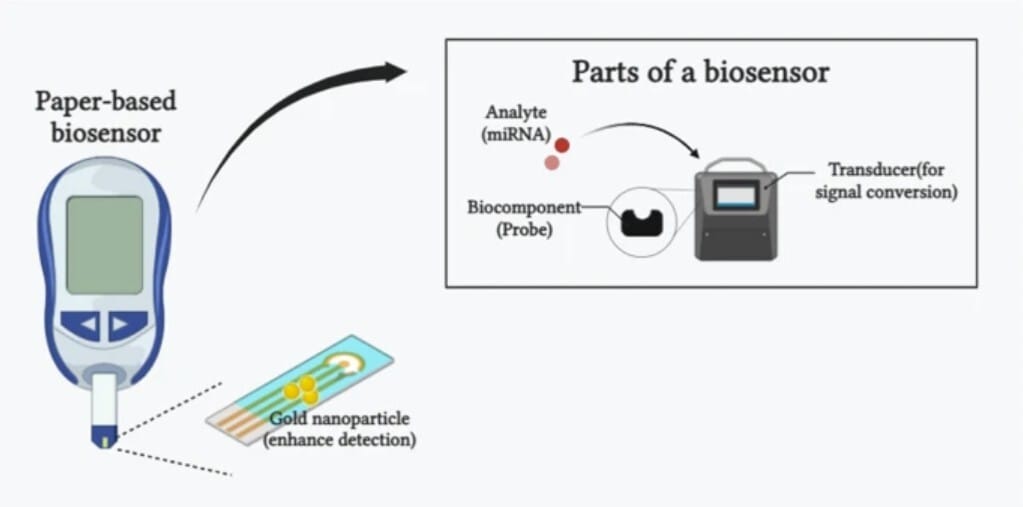
Paper Biosensor for Point of Care Testing of PCa
2026: The Most Important Papers 01/29 - 02/04
This study looks at whether advanced ultrasound combined with artificial intelligence (AI) can reliably detect clinically significant prostate cancer, without relying on MRI. Researchers used a sophisticated form of 3D multiparametric ultrasound that captures not just anatomy, but blood flow patterns and tissue stiffness. They then trained a deep-learning model using prostatectomy specimens as the reference standard, which is about as rigorous as it gets.
In a large, multicenter group of 327 men, the AI system correctly identified clinically significant prostate cancer with high accuracy, performing just as well in a separate external group of patients. The takeaway is simple: ultrasound, when used quantitatively and paired with AI, may offer a far more accessible and cost-effective way to find meaningful prostate cancer early, without defaulting to MRI. This is especially important as we try to keep diagnosis after a rising PSA as minimally invasive as possible.
For a long time, once PCa spread, the options were pretty limited. The focus was almost entirely on systemic therapy, usually hormone deprivation and anything local was mainly about symptom relief. According to this review, much of that thinking has changed. With PSMA-PET imaging, we’re now seeing metastatic disease earlier and with far more clarity than we ever could before. And once you can see it, you have to rethink how it’s treated.
What this paper makes clear is that for some men, treating the prostate itself and sometimes even individual metastatic spots, can actually change the trajectory of the disease. That’s a huge shift, particularly those men with low metastatic burden or what we call oligometastatic disease. It doesn’t mean this approach is right for everyone, but it does mean metastatic PCa is no longer treated with a single arrow. And for your loved ones, that nuance can open doors that simply didn’t exist before.
This paper caught my attention right away because it involves something I’ve spent much of my professional life working with: lasers. We always talk about holmium lasers when we’re discussing lasers used for surgery (non-dental), but I honestly never knew what they were for. Specifically, the article looks at holmium laser enucleation of the prostate, or HoLEP, in men over the age of 80.
Historically, this group has often been steered away from surgery because of age, blood thinners or overall medical complexity and many end up living with long-term catheters instead. What makes this study so compelling is the sheer scale and experience behind it. Over 16 years, more than 1,800 octogenarians were treated at a high-volume center and when the authors compared them carefully to younger men with similar risk factors, the outcomes were remarkably similar.
In plain terms, age alone didn’t translate into higher bleeding risk, more transfusions or major complications. The laser did what good laser technology is supposed to do: precise tissue removal with excellent hemostasis, even in patients most surgeons worry about.
This study really grabbed me because it sits right at the intersection of two things I care deeply about: avoiding overtreatment and using technology thoughtfully. It looks at a novel cooled laser focal therapy device designed to treat only the cancer inside the prostate, rather than the entire gland. The idea is simple but powerful: if we can precisely ablate the tumor we see on MRI, why accept the collateral damage that often comes with whole-gland surgery or radiation? In this early phase II trial, 100 men with localized, intermediate-risk prostate cancer underwent a day-procedure laser treatment, guided by MRI and real-time temperature monitoring. At three months, 84% had no clinically significant cancer remaining in the treated zone, with relatively small changes in urinary and sexual function. This is early data, and short-term by design, but it shows how far focal, image-guided laser therapy has come — and how much more refined it’s becoming.
PCa isn’t one single disease state and this paper does a good job explaining why that is important. Tumors are often made up of multiple subclones and a single biopsy or blood test can miss what’s actually driving the disease. The authors walk through how epigenetic changes (turning genes on and off) and liquid biopsy tools give us a way to see cancer biology more dynamically.
What I appreciated most is that this isn’t just hype. The paper is very clear about what’s ready for prime time, what’s useful in specific situations and what still needs validation. Used thoughtfully, these tools can reduce unnecessary biopsies, refine risk assessment and help tailor treatment decisions. They tend to work best when layered on top of imaging, pathology and clinical judgment.
This review addresses a problem with PCa care: monitoring PSA works, until it doesn’t. Especially in that gray zone where numbers don’t clearly point one way or the other. What this paper explores is the growing potential of paper-based biosensors as point-of-care diagnostic tools for PCa. These are low-cost, disposable tests that can be run outside of a traditional lab and, in some cases, detect biomarkers at levels below what standard PSA testing can reliably pick up.
By combining paper substrates with nanomaterials and modern sensing techniques, these devices deliver sensitive, quantitative results quickly and with minimal infrastructure. This is still an emerging field, but I love the direction of smarter diagnostics that are more accessible, less invasive and better suited for early detection and monitoring than what we rely on today.
OTHER NEWS
A few helpful comments let me know that the bullets aren’t really necessary, so I’ve removed the bullets. I think the content is still strong and way easier to read in a single session.
PLEASE SHARE with others who may benefit from the work we’re doing 🙂
And, THANK YOU!!